In his brief tenure as director of the Eli and Edythe Broad Center for Regenerative Medicine and Stem Cell Research at USC, Andrew McMahon has published three articles, in two key areas of his research, that give insight to both the research that is being carried out at the center and the critical role basic science plays in developing 21st-century medical breakthroughs.
One of the articles, published in Developmental Cell in September, explained McMahon’s most recent research on kidney regeneration.
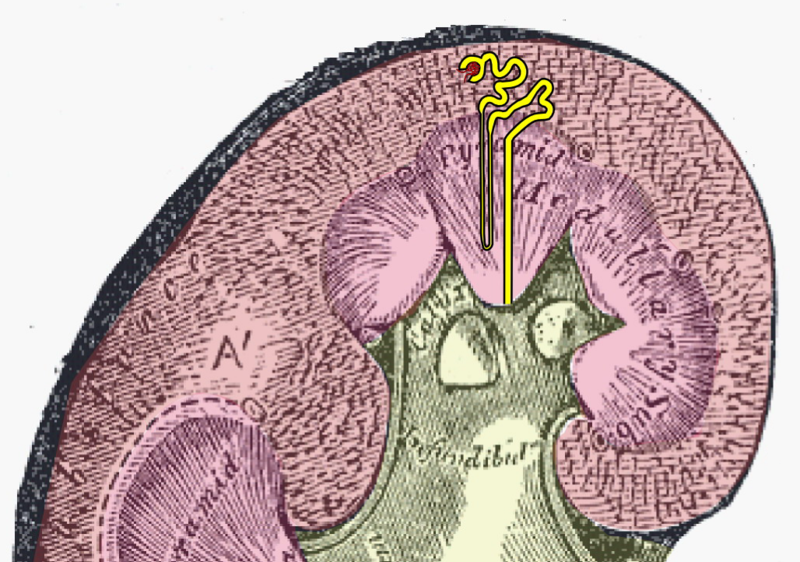
In the article, McMahon and a team of researchers describe the elaborate interplay of reactions that must occur for the body to start building nephrons, the name of the million or so long tubes that are the building blocks of the kidney.
Prior to the publication of this piece, scientists had known that a progenitor cell, defined by expression of the Six2 gene, was critical for the creation of nephrons. What they set out to explain was the precise way in which these cells renew and undergo a process called differentiation, initiating formation of the nephron—an important but poorly understood process.
Not all systems in the body regenerate in the same way. And across the field of stem cell research, scientists are trying to tease out the delicate interplay between the cells known to give rise to organs and proteins such as transcription factors that facilitate that change.
“An important strategy in regenerative medicine is to understand normal mechanisms that generate cell types and harness those mechanisms to regenerate parts of the body,” explained McMahon, who also holds the title of W. M. Keck Provost Professor of Stem Cell Biology and Regenerative Medicine at the Keck School of Medicine of USC.
This research advances the understanding of the interplay of protein binding to DNA targets that must take place in order for the body to start building a kidney. That information, said McMahon, brings science much closer to the point of being able to develop treatments for diseased or damaged kidneys.
Two other recent publications by McMahon both focus on a type of signaling pathway — called the Hedgehog pathway — that hark back to research McMahon began two decades ago on nerve cells.
His initial research on the relationship between nerve cells and certain brain diseases led to research on the Hedgehog pathway, which instructs which type of nerve cells form, and where. It also appears to play a role in the development of certain types of cancerous tumors including the most common brain cancer in children, medulloblastoma, and basal cell carcinoma — a highly prevalent though usually non-life-threatening skin cancer.
Both of the recent publications came out of ongoing research to understand those conditions that exist when the Hedgehog pathway begins developing tumor cells and to find ways to modify them in an effort to halt the development of tumors.
The first of the articles, published in ACS Chemical Biology, examines the role of a protein, dubbed Smoothened (Smo), which acts like an on-off switch in the pathway.
The research team screened about 5,600 drug-like molecules for interactions that would inhibit the role of Smo in the pathway. The painstaking work identified a range of new compounds that control the pathway and potential leads for anti-tumor agents.
“We found some promising compounds that we are going to be testing,” said McMahon.
The findings in the other paper involving the Hedgehog pathway were a surprise to the researchers, he noted.
In the course of screening drugs, the team stumbled across a reaction they did not anticipate, the findings of which were published in Chemical Biology in August.
They discovered that glucocorticoids, a class of hormones that are commonly used as anti-inflammatory drugs, stimulate movement of Smo to a part of the cell that enhances signaling.
The unexpected interplay between these pathways suggests, said McMahon, that the presence of high concentration of glucocorticoids may modify the effects of the newly emerging drugs that are treating Hedgehog pathway-related cancers.
