New study suggests that neural crest cells are reprogrammed into tumor-forming cells, reshaping the understanding of this childhood cancer.
For decades, scientists have been puzzled by two enduring mysteries around Ewing sarcoma. Why does this aggressive bone and soft tissue cancer mainly affect children and adolescents? And why do its tumor cells appear so primitive, showing features of multiple different cell types?
Now, Children’s Hospital Los Angeles researchers may have found answers to these questions. Their newly published study, a close collaboration with the Keck School of Medicine of USC, provides the first in vivo genetic evidence that Ewing sarcoma may originate from neural crest cells—flexible embryonic cells that normally give rise to neurons, glial cells, and pigment cells.
The team showed that a common mutation in this cancer—the EWSR1::FLI1 fusion oncogene—can reprogram neural crest cells into a mesoderm-like state, adopting features of bone- and muscle-forming cells. Results were published in Cell Reports – Opens in a new window.
“This is an exciting step forward in Ewing sarcoma research,” says James Amatruda, MD, PhD, Director of the Cancer and Blood Disease Institute at Children’s Hospital Los Angeles and senior author of the study. “By understanding where and how this disease begins, we open the door to developing more effective and less-toxic treatments.”
Oncogene hijacks development
Scientists have known for more than 30 years that the EWSR1::FLI1 fusion is the driver of Ewing sarcoma. But they didn’t know which specific cells it could transform into cancer, and they lacked reliable research models of the disease. Those gaps have stalled progress in finding new and better therapies.
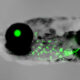
To study this cancer’s earliest steps, Dr. Amatruda’s lab published the first genetic zebrafish model of Ewing sarcoma in 2022. Zebrafish embryos are transparent and develop outside the mother, allowing the team to characterize the earliest stages of Ewing sarcoma and track fluorescently tagged tumor cells in real time.
In this latest study, researchers used the zebrafish model to switch on the EWSR1::FLI1 fusion in different cell types. Most cells died. But neural crest cells were the exception. They not only survived, but they were reprogrammed into a mesoderm-like state, setting the stage for tumor initiation.
The work was the result of a collaboration between Dr. Amatruda’s team at CHLA and the laboratory of Gage Crump, PhD, Professor and Vice Chair of Stem Cell Biology and Regenerative Medicine at USC. Elena Vasileva, PhD, a postdoctoral fellow at CHLA, was the study’s first author.
The team found that the oncogene doesn’t just push cells down the wrong path—it co-opts the same signaling pathways the cells use in normal development. This forces the neural crest cells into an “in-between” state that fuels uncontrolled growth.
“It was remarkable to see how these pre-tumor cells changed their behavior and characteristics, contributing to tumor development later on,” Dr. Vasileva says. “Even more surprising was that the reprogrammed cells appeared to hijack normal developmental programs, such as those responsible for limb development.”
Embryonic cells at a crossroads
Because neural crest cells are only present during early development, the findings help explain why Ewing sarcoma affects children and adolescents, but not older adults. The cells’ reprogramming may also account for the puzzling mixed appearance of Ewing sarcoma cells under the microscope.
“The precancer cells seem to be caught at a crossroads of multiple potential cell fate decisions,” Dr. Vasileva explains. “By understanding these reprogramming trajectories, we may be able to uncover new vulnerabilities of cancer cells and identify new therapeutic targets.”
Next steps for Ewing sarcoma research
By pinpointing a likely cell of origin for Ewing sarcoma, the researchers can now explore new questions: How do these reprogrammed cells fuel tumor growth? What signals do they hijack to spread? And how might those processes be stopped?
The zebrafish model gives the team a powerful tool to study how tumor cells evade the immune system and why they metastasize so aggressively. Researchers are also investigating how these cancer cells interact with their surrounding microenvironment—the network of cells and proteins that tumors hijack to survive.
“The more we understand about how Ewing sarcoma begins, the better models we can build to accurately mimic the disease,” Dr. Amatruda says. “The ultimate goal is to find new and less-toxic treatments for this cancer—and improve outcomes for children.”
See how CHLA is advancing care and research for pediatric cancer.